Sometimes a parent sits across from me and says, “Nothing big happened. That’s why I feel crazy for being worried.” Sometimes it’s an adult who says, “My childhood looked fine on paper, so why do I feel so empty?” Those two sentences usually point to the same wound.
You may be here because your child seems oddly shut down, too agreeable, too self-sufficient, or tense in ways you can’t explain. Or you may be the one carrying a low-grade sense that something in you never fully formed. Not dramatic. Not easy to prove. Just there.
That instinct matters.
The Feeling That Something is Missing

A lot of people looking for signs of emotional neglect in childhood aren’t looking for a label. They’re looking for relief. They want someone to tell them they’re not inventing the problem.
If you’re an adult survivor, the feeling often sounds like this. You function. You handle things. People may even describe you as strong. But underneath that competence is a private hollowness, a sense that your emotions don’t fully register until they spill over or go numb.
If you’re a parent, it may look different. Your child doesn’t always melt down. They may do the opposite. They ask for very little. They say “I’m fine” too quickly. They seem mature beyond their years, but not in a peaceful way. More in a way that makes you wonder who taught them not to need.
When the absence is the clue
Emotional neglect confuses people because there may be no sharp memory to point to. No obvious scene. No clean story. Just a pattern of not being emotionally met.
That’s why so many adults minimize it. “My parents provided.” “They weren’t cruel.” “Other people had it worse.” All of that can be true, and something essential can still have been missing.
You don’t have to prove a dramatic childhood to take your own pain seriously.
This is also why parents miss it in real time. We tend to look for loud signs. Aggression. school refusal. broken trust. But a child who’s gone quiet inside can be just as distressed. They’ve learned that showing need doesn’t lead anywhere useful.
Your concern is not overreaction
Research has found that emotional neglect is one of the most common forms of maltreatment, with about 18% of adults worldwide self-reporting it in childhood, according to this meta-analytic review on childhood emotional neglect. Common doesn’t mean harmless. It means many people carry this wound without language for it.
If the phrase “something is missing” hits hard, that’s not random. It often points to a history of not being emotionally known, mirrored, or responded to in ways a child needs for healthy development.
For parents, one of the most protective shifts is learning what emotional availability in everyday family life looks like. Not perfection. Presence. Not constant talking. Accurate emotional contact.
Free Guide
See People Clearly
7 truths that change how you show up. Free guide, sent to your inbox.
No spam. Unsubscribe anytime.
What Emotional Neglect Actually Is and Why It’s Invisible
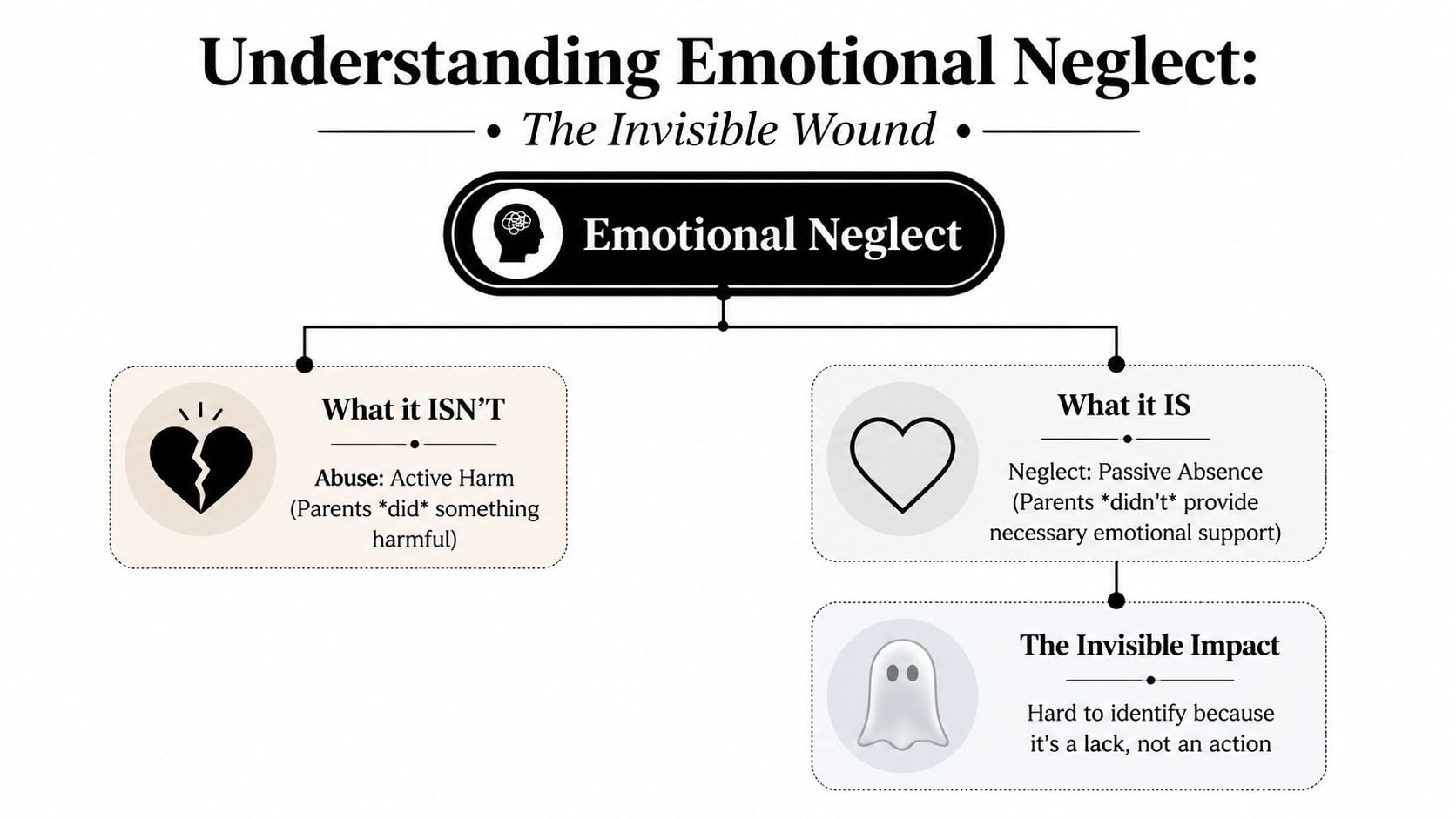
Emotional neglect is not mainly about what a caregiver did. It’s about what they consistently failed to do.
A child needs more than food, shelter, rules, and logistics. They need emotional attunement. Someone who notices their inner state, responds to it with enough care, and helps them make sense of what they feel. When that doesn’t happen, the child doesn’t just feel lonely. The child starts building an identity around the idea that their feelings don’t matter, don’t make sense, or create inconvenience.
It’s an absence, not always an event
Abuse is often easier to identify because it involves active harm. Neglect often hides in omission. No comfort after distress. No curiosity about your inner world. No help naming feelings. No repair after emotional disconnection.
That’s why this wound can stay invisible for years.
A plant can sit in a nice pot in a safe house and still wither if it never gets sunlight. Many emotionally neglected children grow up in homes that looked decent from the outside. The missing ingredient wasn’t structure. It was warmth, reflection, and emotional response.
Why survivors doubt themselves
Children are wired to protect their bond with caregivers. So when a caregiver can’t meet emotional needs, the child rarely concludes, “My parent lacks attunement.” The child concludes, “Something about me must be too much, too sensitive, too needy, or too unimportant.”
That conclusion can follow you for decades.
Practical rule: If your first instinct is to dismiss your own emotional experience, that pattern itself may be part of the injury.
Parents need to hear something important here. Emotional neglect doesn’t require bad intent. A loving parent can still be emotionally unavailable. A stressed parent, depressed parent, traumatized parent, rigid parent, or high-functioning but emotionally shut-down parent can miss a child’s internal world without meaning to.
That doesn’t make you evil. It makes you responsible.
If you’ve caught yourself wondering whether being emotionally overwhelmed makes you a bad parent, the better question is this. Can you notice the gap and start repairing it? That’s where change begins.
The Lifelong Echo of an Unseen Wound
The deepest damage from emotional neglect is not just hurt feelings from long ago. It’s the internal operating system a child builds to survive it.
When caregivers repeatedly miss, dismiss, or flatten a child’s emotions, the child adapts. They may become anxious and cling to connection. They may become avoidant and stop reaching altogether. They may learn to scan constantly for rejection, suppress emotion under stress, or assume that closeness is unreliable.
The message becomes identity
Children don’t naturally know what their feelings mean. They learn through relationship. A responsive adult helps them organize distress, joy, anger, shame, fear, and disappointment into something understandable. Without that help, emotions feel confusing or unsafe.
Over time, the child often absorbs messages like these:
- My needs burden people
- Strong feelings should be hidden
- I should handle everything alone
- If I need comfort, I’m weak
- If someone pulls away, it must be my fault
Those beliefs don’t stay in childhood. They show up in adult friendships, marriage, parenting, work, and health.
Why this affects depression and attachment
One clinical study of adults with anxiety and depressive disorders found that 45.1% reported childhood emotional neglect, making it the most commonly reported form of maltreatment in that group, and it correlated strongly with depressive symptom severity (r = -0.28, p < 0.001), as noted in the earlier research on childhood emotional neglect.
That finding fits what I see in practice. Adults who grew up emotionally unseen often don’t just feel sad. They feel structurally disconnected from themselves. They struggle to identify what they feel, ask for what they need, or believe that support will hold.
If nobody helped you carry emotion when you were small, your nervous system often learns that emotion itself is a problem.
This is why emotional neglect can produce such confusing adult symptoms. Not only loneliness, but self-doubt. Not only conflict in relationships, but difficulty even knowing what you want. The original wound was relational, so the echoes tend to appear anywhere dependence, trust, or vulnerability are required.
How Emotional Neglect Shows Up in Real Life
Most articles on signs of emotional neglect in childhood give a generic list. That’s not enough. The same wound can look compliant in one child, aggressive in another, and “mature” in a third.
The useful question is not, “Does this child look troubled in an obvious way?” The useful question is, “How has this child adapted to not feeling emotionally held?”
The early pattern often starts in attachment
In infancy, neglect can disrupt caregiver attachment and is linked with cognitive delays, social withdrawal, and a two-to-three times higher risk of internalizing disorders like anxiety later in life, according to this review on assessing emotional neglect in infants.
That doesn’t mean every quiet child is neglected. It does mean chronic emotional misattunement leaves a developmental footprint.
Signs by developmental stage
| Stage | Common Signs at Home | Common Signs in School/Socially |
|---|---|---|
| Infancy | Limited seeking of comfort, flat or hard-to-read reactions, difficulty settling, weak back-and-forth emotional engagement with caregivers | Reduced social interest, less interactive play, withdrawal around unfamiliar adults or children |
| Early childhood | Excessive compliance, frequent aggression, passivity, demanding behavior, seeming “too independent,” caring for siblings in a parent-like way, infantile behavior when stressed | Trouble joining play, clinging or avoiding peers, big reactions to minor setbacks, difficulty trusting adults |
| Middle childhood | Hiding feelings, saying “I’m fine” when clearly upset, strong shame after mistakes, low frustration tolerance, little spontaneous sharing, acting older than age emotionally | Social withdrawal, perfectionism, fear of criticism, conflict around boundaries, trouble asking for help |
| Adolescence | Fierce self-reliance, emotional shutdown, irritability, exhaustion, secret sadness, discomfort with affection, pushing away support | Isolation, unstable friendships, sensitivity to rejection, people-pleasing, risk-taking or total disengagement |
A pattern matters more than any single sign. One rough week doesn’t equal neglect. Ongoing emotional nonresponse does.
What parents often misread
Parents often misread the “easy child.” The child who never asks for much. The child who handles disappointment alone. The child who gives a shrug instead of an opinion. That can look like resilience. Sometimes it’s resignation.
Watch for these behavioral clues:
- Hyper-independence: The child avoids relying on anyone, even when help is available.
- Role reversal: The child manages siblings, comforts adults, or acts like the emotional stabilizer in the house.
- Mismatch reactions: A tiny correction brings panic, anger, or shutdown because the child already expects emotional disconnection.
- Thin self-expression: The child can describe events but not inner experience.
A neglected child doesn’t always say, “No one sees me.” More often they build a personality around not needing to be seen.
The Body’s Scorecard Unseen Neglect

This is the part many people miss. Emotional neglect has a physical signature.
When a child’s emotions aren’t welcomed, explained, or soothed, the body still has to do something with that activation. The feelings don’t vanish. The nervous system contains them. That can turn into chronic tension, shallow breathing, fatigue, stomach issues, headaches, restlessness, or a numb, disconnected relationship to the body itself.
What I look for clinically
I pay close attention to jaw tension, raised shoulders, collapsed posture, overcontrolled breathing, and the child or adult who says “I don’t know” while their body is screaming the answer. A lot of people learned early that naming emotion didn’t help, so their body became the storage unit.
That’s one reason emotional neglect gets misread. The person may present with burnout, sleep trouble, unexplained pain, or constant exhaustion and never connect it to old emotional deprivation.
The body remembers what the mind minimizes
Somatic therapy practitioners report that 70-80% of clients presenting with trauma-related physical symptoms also report histories of childhood emotional neglect when probed, linking suppressed emotion to a frozen physical stress response, according to Blue Knot’s discussion of emotional neglect and trauma patterns.
That doesn’t mean every tense body tells the same story. It does mean the body is often telling part of the story before the person has language for it.
A few common somatic clues:
- Chronic guarding: Tight neck, shoulders, jaw, chest, or belly.
- Fatigue without clarity: You’re tired, but rest alone doesn’t seem to solve it.
- Low interoception: You struggle to identify hunger, stress, sadness, anger, or overwhelm until they’re intense.
- Stress collapse: After pushing hard, your body drops suddenly into shutdown, illness, or emotional flatness.
When a child can’t safely express distress, the nervous system often shifts from communication to containment.
For parents, this matters because some children show emotional neglect through the body before they show it in words. They get clingy during conflict. They go rigid when corrected. They complain of stomachaches on high-stress days. They look “dramatic,” but their body may be signaling what nobody has helped them translate.
The Path Forward How to Begin Healing
Once you can see the pattern, the work changes. You stop arguing with reality and start building capacity.
That matters because neglect often moves through families subtly. One study found a child’s emotional neglect score increased by 0.3 points for every ACE their father had experienced, according to this research on intergenerational transmission of emotional neglect. The point isn’t to blame fathers. The point is to see that unprocessed pain gets passed through behavior, silence, and nervous system habits unless someone interrupts it.
If you’re an adult survivor
Start small. Grand insights are less useful than repeatable contact with yourself.
-
Name one feeling before you explain it away
Don’t begin with a full life review. Begin with a sentence like, “I feel hurt,” or “I feel shut down,” or “I feel pressure in my chest and I think it’s fear.” If all you can notice at first is the body, start there. -
Track the moments you disappear
Notice when you go blank, become overly helpful, overwork, withdraw, or say “it’s fine” too quickly. Those are often protection strategies, not personality flaws. -
Practice corrective self-talk
Try language that counters the old script.
“My feelings make sense.”
“Needing support is not failure.”
“I can pause before I perform competence.” -
Use therapy with a clear target
Not every therapist works well with emotional neglect. Look for someone who understands attachment, emotional regulation, and body-based responses. Modalities such as Emotion-Focused Therapy, Somatic Experiencing, and practical skills drawn from CBT can help if they’re applied to the underlying issue, not just surface symptoms. If you want a grounding place to start, these cognitive behavioral therapy techniques for noticing patterns and shifting reactions can support the early work.
For the therapy option specifically, the access friction has dropped a lot in the last few years. Online platforms like Talkspace can match you with a licensed therapist usually within 24 hours, work in all 50 states, accept most major insurance, and let you message your therapist between sessions when something comes up that you don’t want to forget. I mention them by name because they’re the platform I’d point a student or coaching client to today — the path from “I think I need help” to “I’m in a session” is short enough to actually walk.
If you’re a parent trying to break the cycle
Children don’t need perfect emotional attunement. They need enough of it, often enough, with repair when you miss.
Try these moves in real life:
-
Replace fixing with joining
Instead of “You’re okay,” try “That was frustrating, wasn’t it?”
Instead of “Don’t be so sensitive,” try “I can see that hit hard.” -
Ask about inner experience, not just events
“What happened at school?” matters less than “What was that like for you?” -
Slow down during conflict
A dysregulated child can’t absorb a lecture. Regulate first. Consequences can wait a minute. Connection can’t. -
Watch the body while you listen
If your child’s shoulders rise, face goes flat, or posture collapses, you’re getting useful information. Stay curious instead of pushing harder.
Repair beats perfection. A parent who says, “I missed you there. Try again, I’m listening now,” gives a child something powerful.
What doesn’t work
A few things reliably fail.
- Logic before connection: Explaining why a child shouldn’t feel what they feel usually drives them further inward.
- Performative reassurance: “Of course you can talk to me” means little if your body, tone, or pace says the opposite.
- Overpraising independence: Some children need help being allowed to need.
- Turning insight into blame: Understanding the pattern should increase responsibility, not shame.
Healing starts when emotional reality becomes speakable, tolerable, and shared.
You Can’t Heal What You Don’t See
Emotional neglect hides in plain sight because it often looks like nothing happened. That’s exactly why so many people miss it.
Seeing it clearly isn’t an accusation. It’s a form of relief. You stop calling yourself broken for having needs. You stop calling your child difficult for showing stress in ways you didn’t recognize. You start reading the pattern accurately.
Some parents who neglected emotionally were neglected themselves. That can explain the gap. It cannot close the gap for you. Only awareness, repair, and practice can do that.
If this article helped you put language to something you’ve felt for a long time, hold onto that. Clarity changes what action becomes possible. Once you can see the wound, you can respond to it differently. In yourself. In your child. In the next conversation that matters.
A note on affiliates: This article includes affiliate links to platforms I’ve vetted and would recommend to my own clients and students. If you start with a recommended service through a link here, I may earn a small commission — at no extra cost to you. I only mention what I’d actually point you to in person. The recommendation comes first; the relationship is disclosed second.